Project 3: providers key moments study
The results and the modalities of this study have been modified in order to protect the confidentiality of Centene’s information.
Overview
Recognizing gaps in understanding the provider experience, Centene launched a qualitative research study to identify the key “moments that matter” across the provider journey.
The initiative surfaced critical friction points, particularly in contracting and claims, and shifted internal priorities toward provider-led, evidence-based experience improvements. The insights informed a new strategic roadmap for the UXR team and cross-functional stakeholders, shaping the future direction of the Providers’ experience.
The context
Centene is a large healthcare insurance organization that works closely with medical providers across the U.S. Providers interact with Centene daily on activities such as contracting, billing, claims, and administrative coordination.
While Centene continuously evolves its systems and processes, leadership identified a gap in deep, experience-led insight into how providers perceive and navigate their relationship with Centene, particularly compared to other payors.
This research initiative aimed to ground future experience improvements in the real, lived experiences of providers
Objective
To gain a clearer understanding of who the providers are, I first needed to better understand::
How providers experience working with Centene day-to-day
Where Centene performs well vs. where friction occurs
How Centene compares to other payors from a provider perspective
Which “moments that matter” most influence trust, efficiency, and
satisfaction

Research goals
Among providers who interact with Centene regularly, the study sought to:
Understand the end-to-end provider experience of working with Centene
Identify key strengths and pain points from the provider perspective
Compare Centene to other payors in terms of ease, clarity, and efficiency
Surface the critical moments that matter that shape the overall relationship
Definition of “Providers”
For the purposes of this project, providers are defined as anyone employed by a provider office or group that is involved in contracting or interacting with Centene on a daily basis. Common non-clinical role titles can include, but are not limited to:
• Office Manager
• Billing Manager
• Claims Director

Research Approach
Methodology
A qualitative research approach mixing attitudinal and behavioral methods was chosen to
capture nuance, emotion, and complexity.
Methods included:
40 in-depth 1:1 interviews - Digital Ethnographic research with provider staff - in 25 States
Including 10 Ethnographic interviews - in site walkthroughs of providers interactions with Centene
Comparative discussions referencing other payors
Thematic synthesis and journey mapping
This approach allowed us to move beyond surface-level satisfaction metrics and uncover why
certain experiences worked or failed.

key research questions
What does a “typical” interaction with Centene look like for providers?
Where do providers feel supported vs. frustrated?
Which processes feel clear, and which feel unnecessarily complex?
How does Centene compare to other payors providers work with regularly?
Which moments disproportionately influence trust, confidence, and effort?
realization of the research
Introduction of the provider to get an understanding of their context and their work
Par vs. term decision-making: Identify the top factors influencing whether providers stay in-network or terminate a health plan contract, how those factors are prioritized, what constitutes a deal breaker, and any recent experiences or considerations around terming.
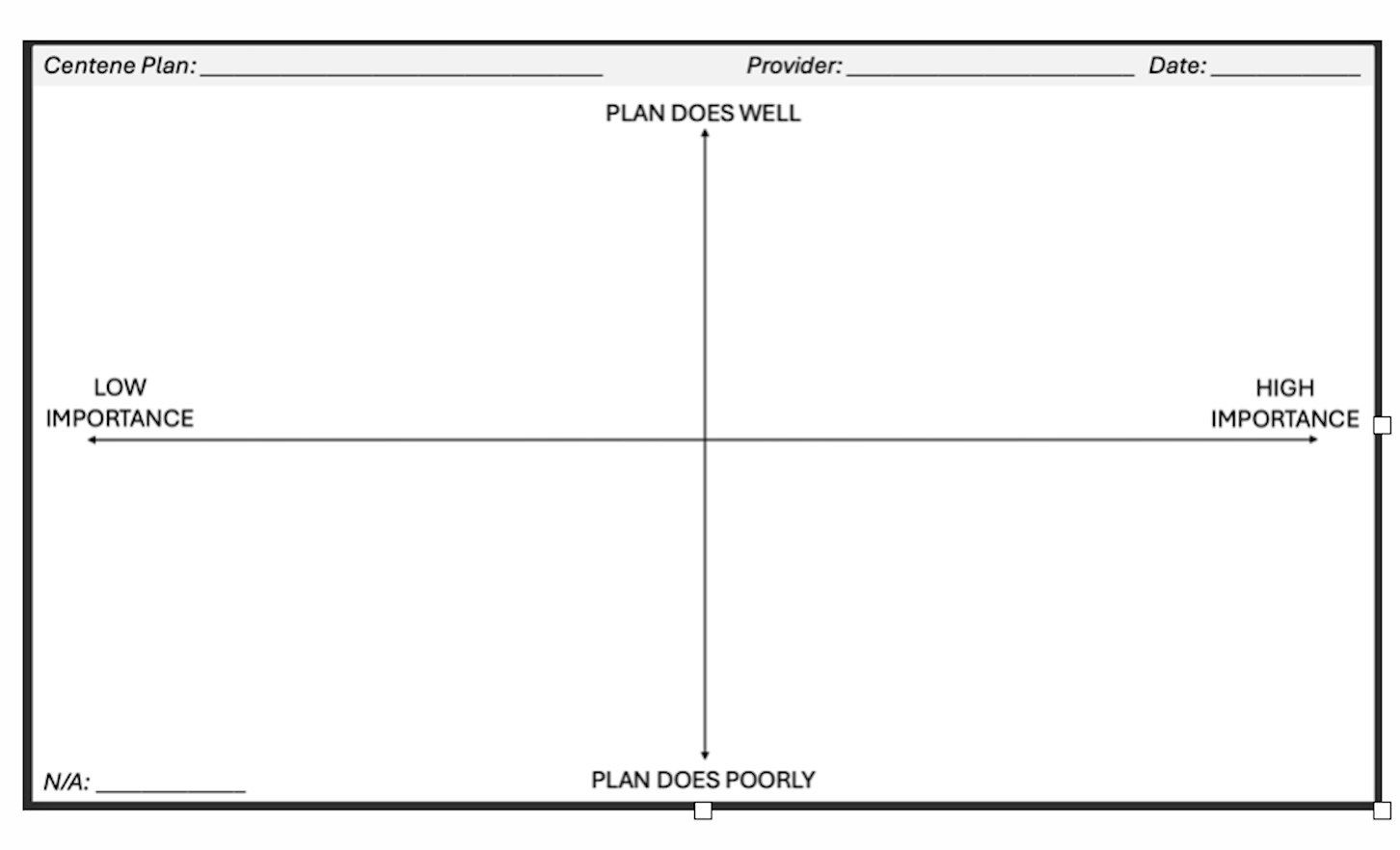
Moments that Matter exercise: Have participants map key health plan interactions on an importance vs. performance matrix for the plan they work with most, to identify strengths, gaps (especially high-importance/low-performance areas), priorities for improvement, and opportunities to learn from better-performing plans.
Channels & platforms: Understand which digital tools (e.g. payor portals, Availity, EMRs) are used for key tasks, which are preferred, what works or doesn’t, and what an ideal single system and future improvements would look like, including who owns tasks not covered.
Performance & partnership: Explore what defines a successful payor–provider relationship, what “best-in-class” health plan support looks like for clinical and quality performance, and where plans can better collaborate to improve provider engagement, satisfaction, and patient outcomes.
Dual-eligible patients: Understand whether and how practices serve dual-eligible patients, the key challenges in managing their care, how health plans currently support these patients, and where additional support or improvements are needed.

Key Insights
The Experience Is Defined by Moments,
Not Systems
Providers didn’t evaluate Centene as a single entity — their
perception was shaped by specific interactions, such as:
• Contract onboarding
• Claims resolution
• Issue escalation
• Responsiveness during time-sensitive moments
A single negative experience in a high-impact moment could
outweigh multiple neutral ones.
Comparisons to Other Payors Were
Constant
Providers naturally benchmarked Centene against other payors
they worked with, especially around:
• Ease of contracting
• Transparency of requirements
• Accessibility of support
• Resolution timelines
Other payors were perceived as “easier” when they reduced
ambiguity — even if their systems were not technically faster.
Clarity and Consistency Matter More
Than Speed
While efficiency was important, providers emphasized:
• Clear expectations
• Consistent information across channels
• Predictable processes
Inconsistencies between portals, documentation, and human
support created friction and eroded trust.
Providers Felt the Burden of System
Complexity
Many providers felt that administrative complexity was shifted onto them, requiring:
• Extra follow-ups
• Manual tracking
• Repeated explanations
This created emotional fatigue and the sense that providers had
to “manage the system” rather than the system supporting them.
IMpact
This research enabled Centene teams to:
Align around a shared understanding of the provider experience
Shift from internal assumptions to provider-led insights for future design and research
Prioritize improvements for the next road map based on impact, not volume
Use provider language and mental models in future design and process work
The findings informed ongoing experience strategy, service design, and cross-functional decision-making.